Rapid multicontrast brain imaging on a 0.35T MR-linac
By: Karen Holzberger, President & CEO of SpinTech MRI
Author(s): Siamak P Nejad-Davarani 1, Niloufar Zakariaei 1, Yongsheng Chen 2, E Mark Haacke 3 4, Newton J Hurst Jr 1, M Salim Siddiqui 1, Lonni R Schultz 5, James M Snyder 6, Tobias Walbert 6, Carri K Glide-Hurst
Journal: Medical Physics
Published: 2020
Read Full Paper: https://pubmed.ncbi.nlm.nih.gov/32434276/
Abstract
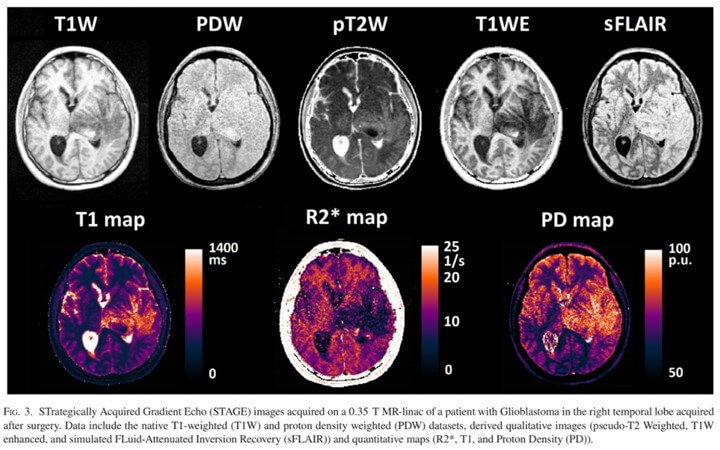
Magnetic resonance-guided radiation therapy (MRgRT) has shown great promise for localization and real-time tumor monitoring. However, to date, quantitative imaging has been limited for low field MRgRT. This work benchmarks quantitative T1, R2, and Proton Density (PD)mapping in a phantom on a 0.35 T MR-linac and implements a novel acquisition method, STrategically Acquired Gradient Echo (STAGE). To further validate STAGE in a clinical setting, a pilot study was undertaken in a cohort of brain tumor patients to elucidate opportunities for longitudinal functional imaging with an MR-linac in the brain.
Method
STAGE (two triple-echo gradient echo (GRE) acquisitions) was optimized for a 0.35T low-field MR-linac. Simulations were performed to choose two flip angles to optimize signal-to-noise ratio (SNR) and T1-mapping precision. Tradeoffs between SNR, scan time, and spatial resolution for whole-brain coverage were evaluated in healthy volunteers.
Data were inputted into a STAGE processing pipeline to yield four qualitative images (T1-weighted, enhanced T1-weighted, proton-density (PD) weighted, and simulated FLuid-Attenuated Inversion Recovery (sFLAIR)), and three quantitative datasets (T1, PD, and R2). A benchmarking ISMRM/NIST phantom consisting of vials with variable NiCl2 and MnCl2 concentrations was scanned using variable flip angles (VFA) (2-60 degrees) and inversion recovery (IR) methods at 0.35 T. STAGE and VFA T1 values of vials were compared to IR T1 values.
As measures of agreement with reference values and repeatability, relative error (RE) and coefficient of variability (CV) were calculated, respectively, for quantitative MR values within the phantom vials (spheres). To demonstrate feasibility, longitudinal STAGE data (pretreatment, weekly, and ~ 2 months post-treatment) were acquired in an IRB-approved pilot study of brain tumor cases via the generation of temporal and differential quantitative MRI maps.
Results
In the phantom, RE of measured VFA T1 and STAGE relative to IR reference values were 7.0 ± 2.5% and 9.5 ± 2.2% respectively. RE for the PD vials was 8.1 ± 6.8% and CV for phantom R2* measurements was 10.1 ± 9.9%. Simulations and volunteer experiments yielded final STAGE parameters of FA = 50°/10°, 1 × 1 × 3 mm3 resolution, TR = 40 ms, TE = 5/20/34 ms in 10 min (64 slices). In the pilot study of brain tumor patients, differential maps for R2* and T1 maps were sensitive to local tumor changes and appeared similar to 3 T follow-up MRI datasets.
Conclusions
Quantitative T1, R2*, and PD mapping are promising at 0.35 T agreeing well with reference data. STAGE phantom data offer quantitative representations comparable to traditional methods in a fraction of the acquisition time. Initial feasibility of implementing STAGE at 0.35 T in a patient brain tumor cohort suggests that detectable changes can be observed over time. With confirmation in a larger cohort, results may be implemented to identify areas of recurrence and facilitate adaptive radiation therapy.

